In a New York Times article, survivors of COVID-19 who have had the disease for weeks to months—termed “long haulers”—describe oral problems they’re experiencing such as “teeth falling out, sensitive gums, teeth turning grey, and teeth cracking.”1 Although many physicians continue to question the direct link between SARS-CoV-2 and oral disease, studies suggest that the mouth might be the most vulnerable area to this virus due to the abundance of the ACE2 (angiotensin converting enzyme) receptor in oral tissue.
The ACE2 receptor has been well-documented to be the target receptor of the SARS-CoV-2 virus and the portal of entry into the human cell.2 A new preprint study found that, compared with other oral tissues, cells of the salivary glands, tongue, and tonsils carry the most RNA linked to proteins that the SARS-CoV-2 virus needs to infect cells.3 Namely, these include the ACE2 receptor and an enzyme called TMPRSS (transmembrane protease, serine 2), which allows the virus to fuse its membrane with that of the host cell and slip inside.
This article will briefly review the top five oral manifestations associated with COVID-19.
No. 1: Gingival inflammation
Bleeding and inflammation in oral tissue have been suggested to be a result of a generalized increase in inflammation due to elevated levels of cytokines and interleukins initiated by the SARS CoV-2 virus. COVID-19 disease severity has been linked to an immune dysregulation, leading to a cytokine storm. Periodontal disease can increase levels of circulating cytokines, particularly interleukin-6 (IL-6), which has been implicated as one of the major interleukins leading to the cytokine storm.4
Periodontal disease is currently being examined as a possible contributing disease toward COVID-19 severity.
No. 2: Xerostomia (dry mouth)
COVID-19 has been suggested to cause dry mouth for a variety of reasons. The most common is mouth breathing by an individual due to mask use. Mouth breathing can desiccate oral tissue especially without frequent hydration. Studies suggest that another biologic mechanism involves viral entry into the salivary glands, which are known to be abundant in the ACE2 receptor.5
Kevin Byrd, DDS, PhD, manager of oral and craniofacial research at the American Dental Association Science and Research Institute, states that novel coronavirus infection of the salivary glands can influence both the quantity and quality of saliva being produced.6
Additional research is needed to identify causal effect, but in the meantime, clinicians should note that xerostomia has been linked to an increase in both caries and candida infections.
No. 3: Oral ulcerations and gingival tissue breakdown
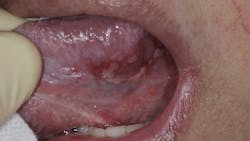
COVID-19 has been associated with vascularity anomalies due to viral damage of blood vessels. William Li, MD, president and medical director of the Angiogenesis Foundation, describes a process whereby the virus gains entry into the endothelial cells that line blood vessels via the ACE2 receptor and damages them, leading to situations of oxygen deprivation. Tissue necrosis, including oral ulcerations, can be the result of vessel damage (figure 1). Ulceration and tissue damage can be further exacerbated by increased inflammation and upregulation in inflammatory markers due to the SARS-CoV-2 virus.7
Case reports have been cited in the literature that show confirmed COVID-19–positive patients having oral ulcerations that were suspected to be caused by the SARS-CoV-2 virus.8
No. 4: Cracked teeth
An article published in September 2020 in the New York Times discussed the phenomena of dentists seeing a tremendous increase in patients presenting to their practices with fractured teeth during the coronavirus pandemic.9 The article cited an increase in bruxism (teeth grinding and clenching) as the mostly likely culprit.
The article specifically examined three COVID-19 pandemic-related factors that could cause an increase in tooth facture from bruxism. First, psychological stress from the pandemic could have a major role in stress-related tooth fracture. Second, poor orthopedic posture from makeshift at-home workstations could lead to bruxism. Finally, sleep deprivation and/or obstructive sleep apnea could result in bruxism and cracked teeth.
No. 5: Loss of taste and smell
A sudden onset in loss of taste (ageusia) and smell (anosmia) are two symptoms that can be the earliest indicators of COVID-19. An average of 47% (up to 80%) of individuals who test positive for COVID-19 can have subjective complaints of taste and smell loss, particularly in cases of asymptomatic or mild disease.10
The mechanism behind this loss is suspected to be viral disruption of cranial nerves 1, 7, 9, and 10, as well as the supporting cells of neural transmission.11 In addition, because the tongue has an abundance of ACE2 receptors, direct viral entry into tongue cells is possible.
Related articles
- Vitamin D deficiency and COVID-19
- Lowering the transmission and spread of human coronavirus with over-the-counter products
- How does COVID-19 affect salivary flow and xerostomia?
- Uncontrolled inflammation: The real problem with COVID-19
Editor’s note: This article originally appeared in Perio-Implant Advisory, a newsletter for dentists and hygienists that focuses on periodontal- and implant-related issues. Perio-Implant Advisory is part of the Dental Economics and DentistryIQ network. To read more articles, visit perioimplantadvisory.com and subscribe at this link.
References
- Yan W. Their teeth fell out. Was it another COVID-19 consequence? The New York Times. November 26, 2020. Updated November 28, 2020. https://www.nytimes.com/2020/11/26/health/covid-teeth-falling-out.html
- Gheblawi M, Wang K, Viveiros A, et al. Angiotensin-converting enzyme 2: SARS-CoV-2 receptor and regulator of the renin-angiotensin system—celebrating the 20th anniversary of the discovery of ACE2. Circ Res. 2020;126(10):1456-1474. doi:10.1161/CIRCRESAHA.120.317015
- Huang N, Perez P, Kato T, et al. Integrated single-cell atlases reveal an oral SARS-CoV-2 infection and transmission axis. medRxiv. 2020;2020.10.26.20219089. doi:10.1101/2020.10.26.20219089
- Tanaka T, Narazaki M, Kishimoto T. Immunotherapeutic implications of IL-6 blockade for cytokine storm. Immunotherapy. 2016;8(8):959-970. doi:10.2217/imt-2016-0020
- Xu J, Li Y, Gan F, Du Y, Yao Y. Salivary glands: potential reservoirs for COVID-19 asymptomatic infection. J Dent Res. 2020;99(8):989. doi:10.1177/0022034520918518
- Lanese N. COVID-19 infects the mouth. Could that explain patients’ taste loss? Live Science. November 2, 2020. https://www.livescience.com/oral-infection-coronavirus-spread.html
- Sampson V, Kamona N, Sampson A. Could there be a link between oral hygiene and the severity of SARS-CoV-2 infections? Br Dent J. 2020;228(12):971-975. doi:10.1038/s41415-020-1747-8
- Sinadinos A, Shelswell J. Oral ulceration and blistering in patients with COVID-19. Evid Based Dent. 2020;21(2):49. doi:10.1038/s41432-020-0100-z
- Chen T. A dentist sees more cracked teeth. What’s going on? The New York Times. September 8, 2020. Updated September 11, 2020. https://www.nytimes.com/2020/09/08/well/live/dentists-tooth-teeth-cracks-fractures-coronavirus-stress-grinding.html
- Agyeman AA, Chin KL, Landersdorfer CB, Liew D, Ofori-Asenso R. Smell and taste dysfunction in patients with COVID-19: a systematic review and meta-analysis. Mayo Clin Proc. 2020;95(8):1621-1631. doi:10.1016/j.mayocp.2020.05.030
- Brann DH, Tsukahara T, Weinreb C, et al. Non-neuronal expression of SARS-CoV-2 entry genes in the olfactory system suggests mechanisms underlying COVID-19–associated anosmia. Sci Adv. 2020;6(31):eabc5801. doi:10.1126/sciadv.abc5801